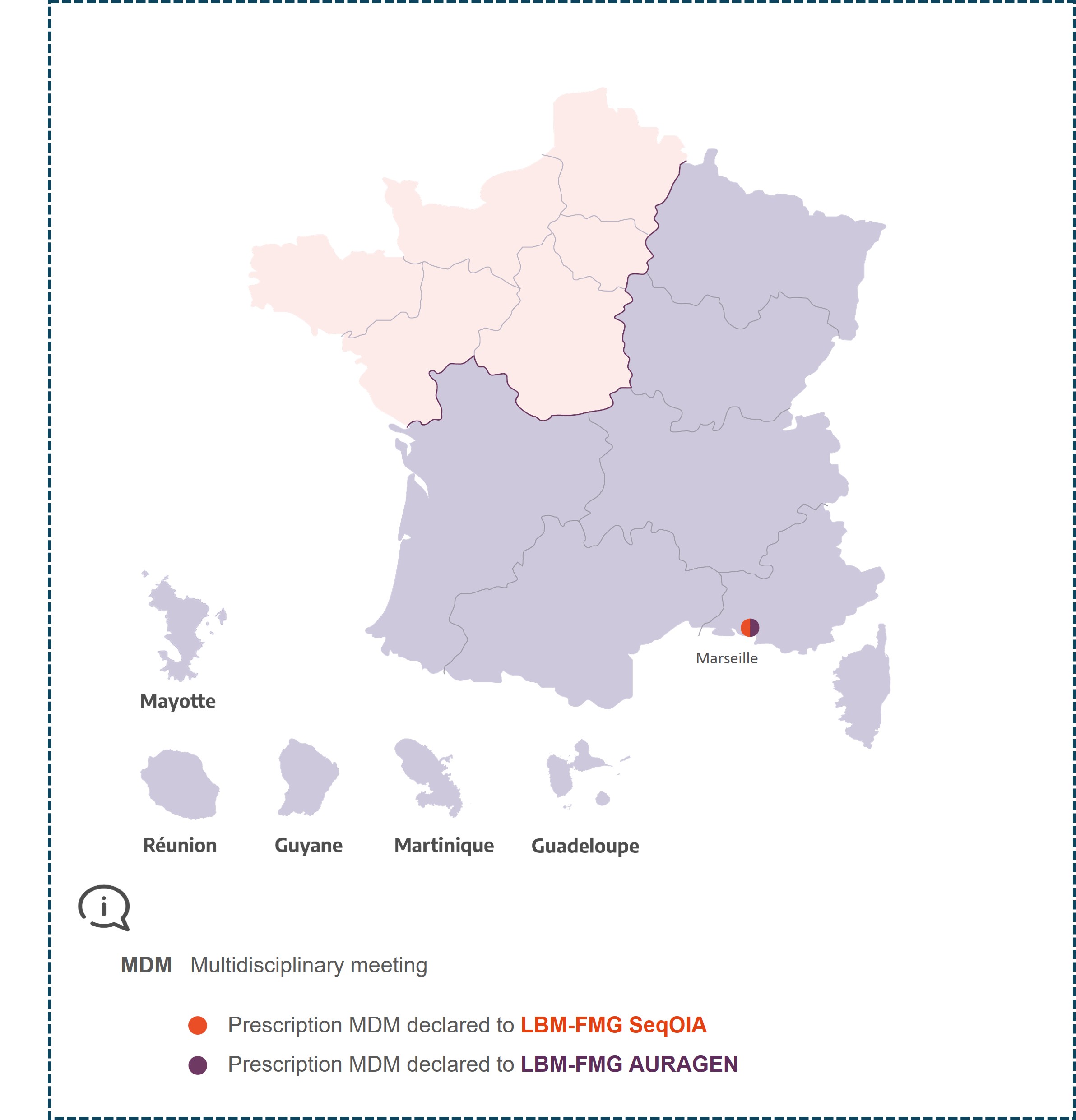
Presentation
The initial diagnosis of dyslipidaemia (six clinical situations currently identified) is based on routine or specialised biochemical investigations, personal or family history, suggestive clinical signs and the use of clinical scores with high discriminatory value. After exclusion of secondary dyslipidaemia, these investigations enable a diagnosis to be made with the implementation of specific treatment. Genetic testing (Sanger approach or gene panel) enables the diagnosis to be confirmed and genetic counselling to be provided.
However, this approach may fail in a number of cases.
Two scenarios can be distinguished:
- Group 1: Situations in which the biochemical profile is pathognomonic of a disease or group of diseases, but genetic testing using a gene panel is negative or partially informative (a single heterozygous mutation in autosomal recessive diseases or in a patient with a homozygous phenotype of a semi-dominant disease): use of High Definition Sequencing to explore deep intronic and regulatory regions of the panel genes as well as genes that have not yet been involved in this nosological context
- Group 2: Situations in which biochemical profiles are atypical: approach using gene panels related to clinical and biological data in first-line, with a lower diagnostic yield than in the first case and therefore more frequent use of WGS
Criteria before considering a discussion in MDM-FMG
- Clinical severity of dyslipidaemia and its complications: use of clinical scores
- Heredity
- Complete phenotyping: specialised analyses already performed
- Exclusion of:
- Secondary forms
- Polygenic forms
- Opinion of the local/regional RCP in favor of a presentation in RCP-FMG
Clinical and biological situations managed in CEDRA that may give rise to discussion in MDM-FMG:
- Mixed Familial hyperlipidaemia (familial combined hyperlipidaemia, dysbetalipoproteinemia and lysosomal acid lipase deficiency, etc.)
- Rare familial hypercholesterolaemia (hyperLDLemia or hyperbetalipoproteinemia) including: complex heterozygous or homozygous hypercholesterolaemia, sitosterolaemia (or phytosterolaemia), cerebrotendinous xanthomatosis, etc.
- Familial heterozygous or homozygous hypobetalipoproteinemia (hypoLDLemia)
- Familial hypoalphalipoproteinemia (hypoHDLemia) including Tangier disease, fish eye diseases, etc.)
- Familial hyperalphalipoproteinemia (hyperHDLemia)
- Familial hypertriglyceridemia including Familial hyperchylomicronemia syndrome (FCS) and Multifactorial hyperchylomicronemia syndrome (MCS), etc.
Genome Sequencing in diagnostic strategy
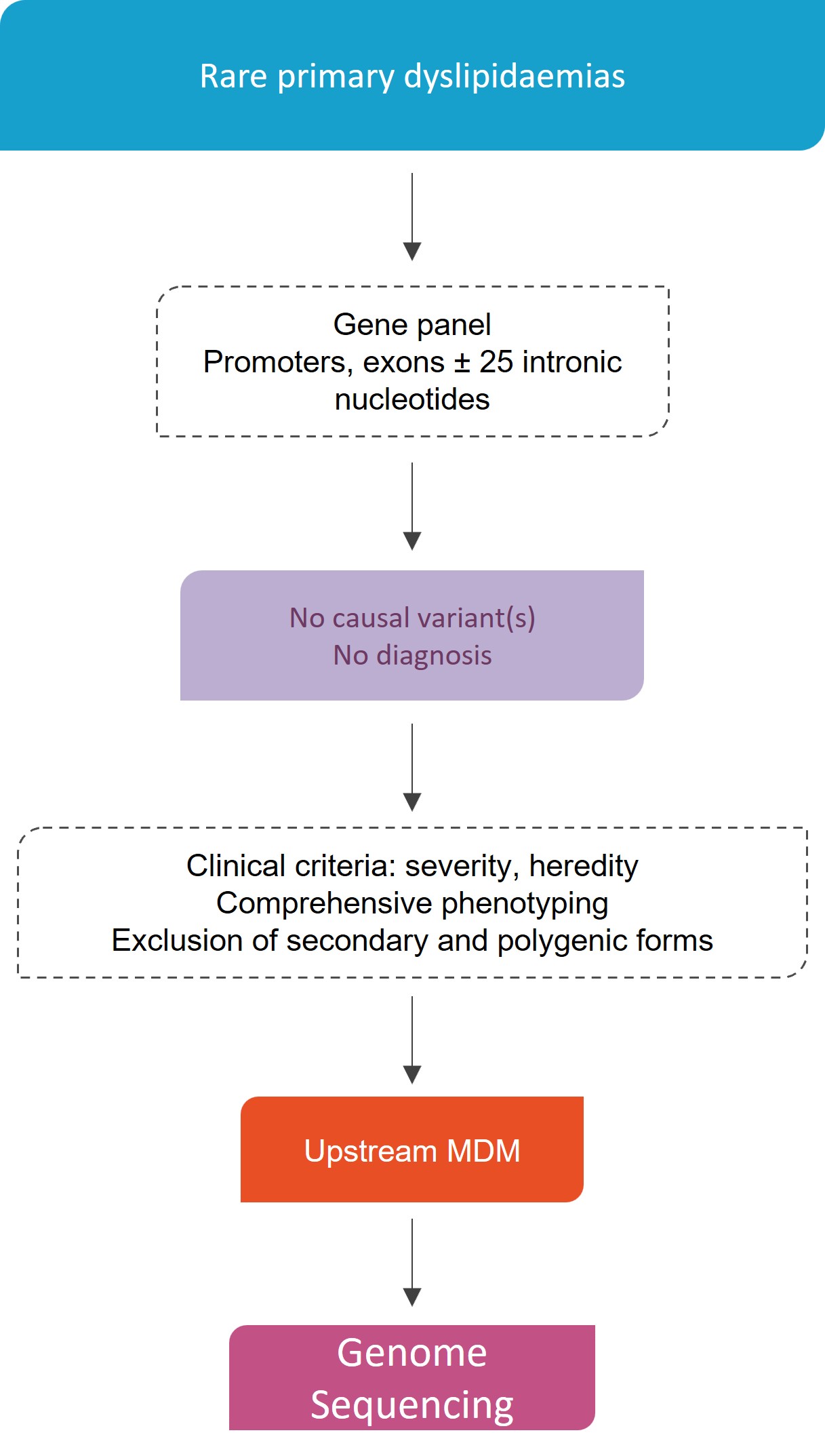
MDM CEDRA (Centre of Expertise in Rare Dyslipidaemias)